Author name:
Olivia Lucianno
In a recent review, researchers from King’s College London grapple with the fact that despite how advanced brain-imaging technologies have become, we still have very limited use for it in diagnosing, monitoring, and treating severe mental illness (SMI).
What imaging methods exist?
The 20th century was filled with exciting advances in technology, particularly in medical imaging. First, the invention of X-ray imaging revealed the rigid bone structures of the skeleton. Next, the ultrasound revealed major structures in the soft tissues of the body. Since then, new techniques have revealed more and more high-resolution detail for the internal structures of organs, most notably the brain.
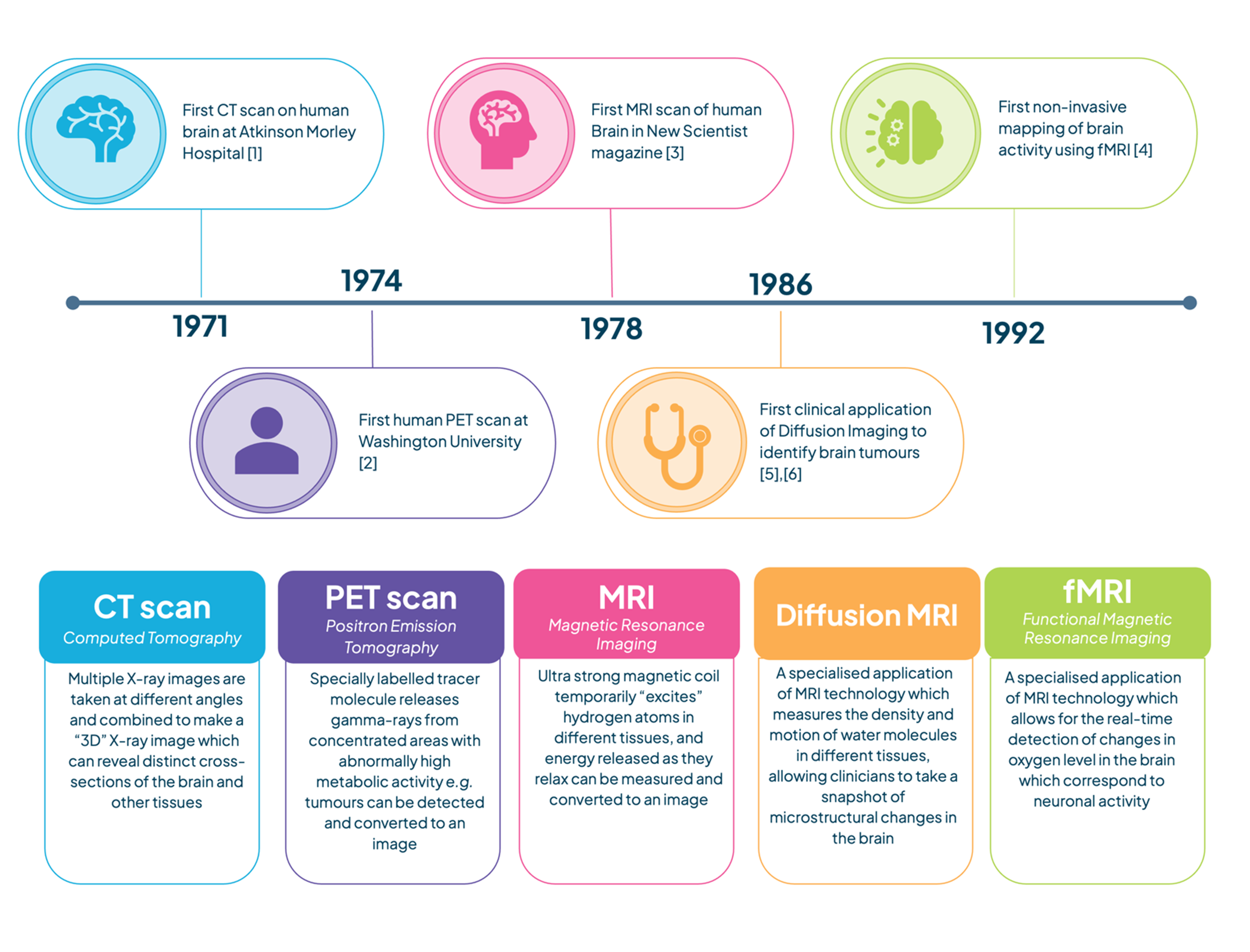
Applications: Expectation vs Reality
Expectation
In the early days of brain imaging, there was a lot of excitement around how it could be used. Clinical applications for identifying stroke or tumour in the brain were adopted early on. However, researchers also anticipated it could be used to diagnose and personalise treatment plans for SMI. This is based on the idea that the human experience is reflected in small changes in the structures of the brain. If only we had the tools to see these changes, then we could truly personalise medical diagnoses and treatment to patients. Somewhat of a tool to see “what your brain says about you”.
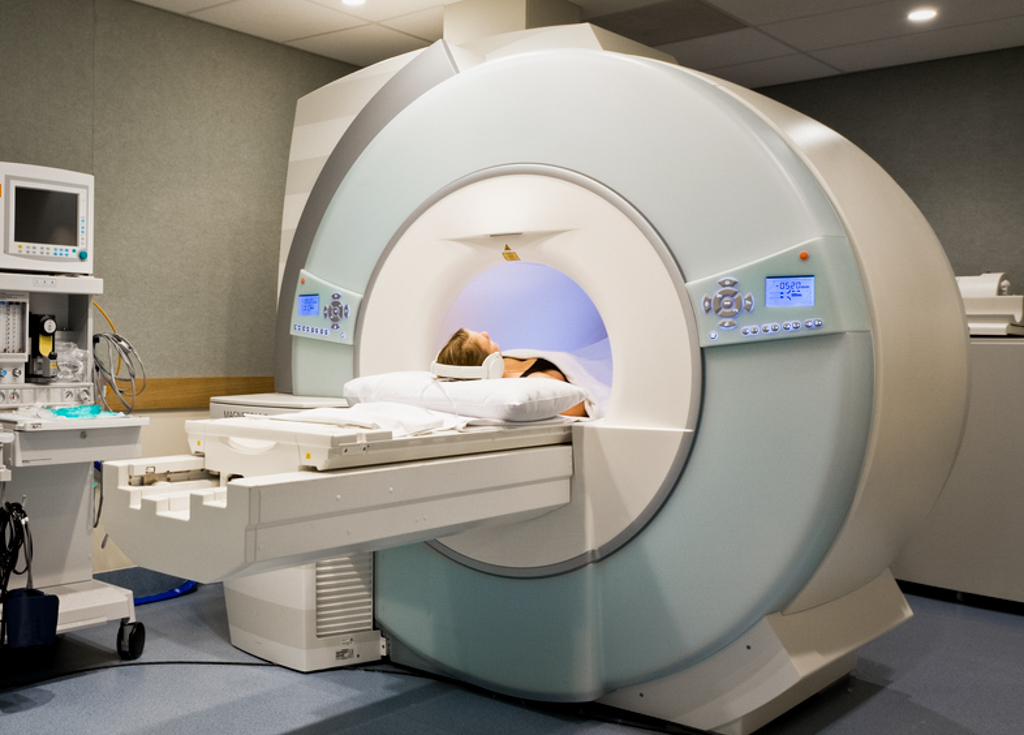
At first, this idea seemed to hold a lot of promise. Structural changes in the brain large and small could be detected even with the earliest imaging technique, the CT scan. Most notably, structural differences in the brains of people with and without a diagnosis of schizophrenia could be identified. Continued research using more advanced imaging techniques allowed us to learn more about fundamental mechanisms in the brain.
Reality
Brain imaging technologies like CT scans and MRI have catapulted our knowledge of basic brain function. They are also an invaluable tool for detecting cancer and stroke early on. However, its use in reliably diagnosing and selecting appropriate treatment plans for SMI is non-existent. There are several reasons for this shortcoming. The first involve technical limitations where still more resolution is needed to trace single neuron activity and relate this to function. The next is a fundamental feature of SMI. Just as everyone’s lived experience of SMI is unique, so too is the structure and function of their brains. This means that currently, there is no single measurable feature that is absolutely linked with a specific mental illness.
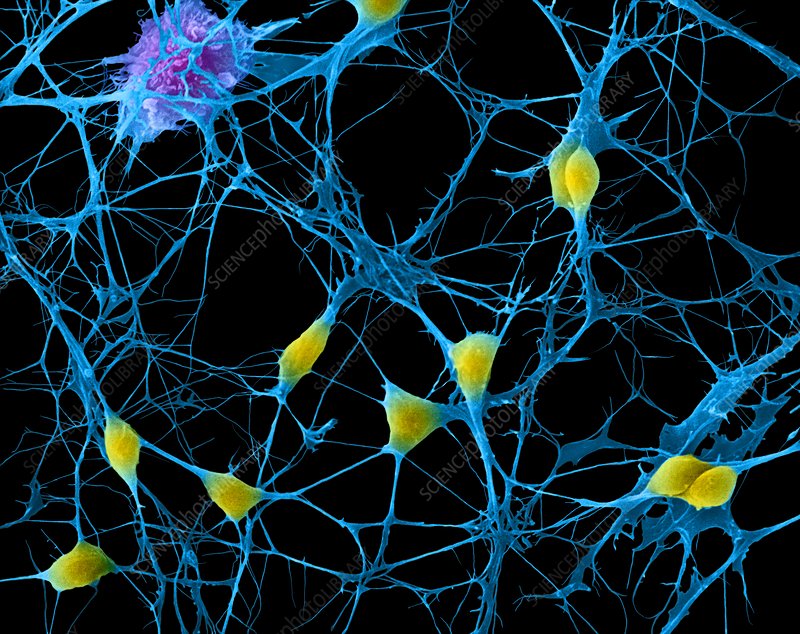
In spite of this, there is still plenty of untapped potential for using this powerful technology in psychiatry. To explore this potential, future research must expand its breadth. Newly recognised factors which contribute to the lived-experience of SMI need to be included in studies involving traditional imaging and drug-based research. Of course, combining this information and finding meaning in it is a massive undertaking. Therefore, it is essential that multi-disciplinary research is prioritised and supported.
What does this mean for people with SMI?
If an expanded approach is used in research, this may pave the way toward more personalised treatment plans. This way, future care that people with SMI may receive may become as multi-faceted and unique as they are as individuals.
Infographic ref list:
[3] Clow, H., & Young, I. R. (1978). Britain’s brains produce first NMR scans. New Scientist, 80(588), b26.
[4] Turner R. (2012). The NIH experience in first advancing fMRI. NeuroImage, 62(2), 632–636.
Published 6 May 2026
Don’t judge a brain by its image - beyond the scanner
In a recent review, researchers from King’s College London grapple with the fact that despite how advanced brain-imaging technologies have become, we still have very limited use for it in diagnosing, monitoring, and treating severe mental illness (SMI).

Published 17 April 2026
ECR Workshop 2026
This workshop is part of MQ and DATAMIND's ongoing series supporting early career researchers in mental health.

Published 17 April 2026
MHP Research Summit 2026
The MHP Research Summit is an annual event for scientists, clinicians and health care professionals to network and share the latest advances in research into severe mental illness
